In recent years, peptide-based therapies have transformed the landscape of weight loss and metabolic health. Among the most promising developments is retatrutide, a novel experimental peptide that is gaining attention for its powerful effects on body weight, glucose regulation, and overall metabolism. Often described as a “next-generation” therapy, retatrutide represents a significant evolution beyond earlier compounds like GLP-1 agonists.
What Is Retatrutide?
Retatrutide (also known as LY3437943) is a synthetic peptide developed by Eli Lilly and currently undergoing advanced clinical trials. It is designed as a triple hormone receptor agonist, meaning it simultaneously activates three key metabolic pathways:
- GLP-1 (glucagon-like peptide-1)
- GIP (glucose-dependent insulinotropic polypeptide)
- Glucagon receptors
This triple-action mechanism is what sets retatrutide apart from earlier therapies. While traditional weight-loss drugs typically target one or two pathways, retatrutide works across three, creating a more comprehensive metabolic effect.
How Retatrutide Works
To understand why retatrutide is so effective, it’s important to break down its mechanism.
- GLP-1 activation helps reduce appetite, slow gastric emptying, and improve insulin secretion.
- GIP activation enhances insulin sensitivity and supports better glucose control.
- Glucagon receptor activation increases energy expenditure and promotes fat breakdown.
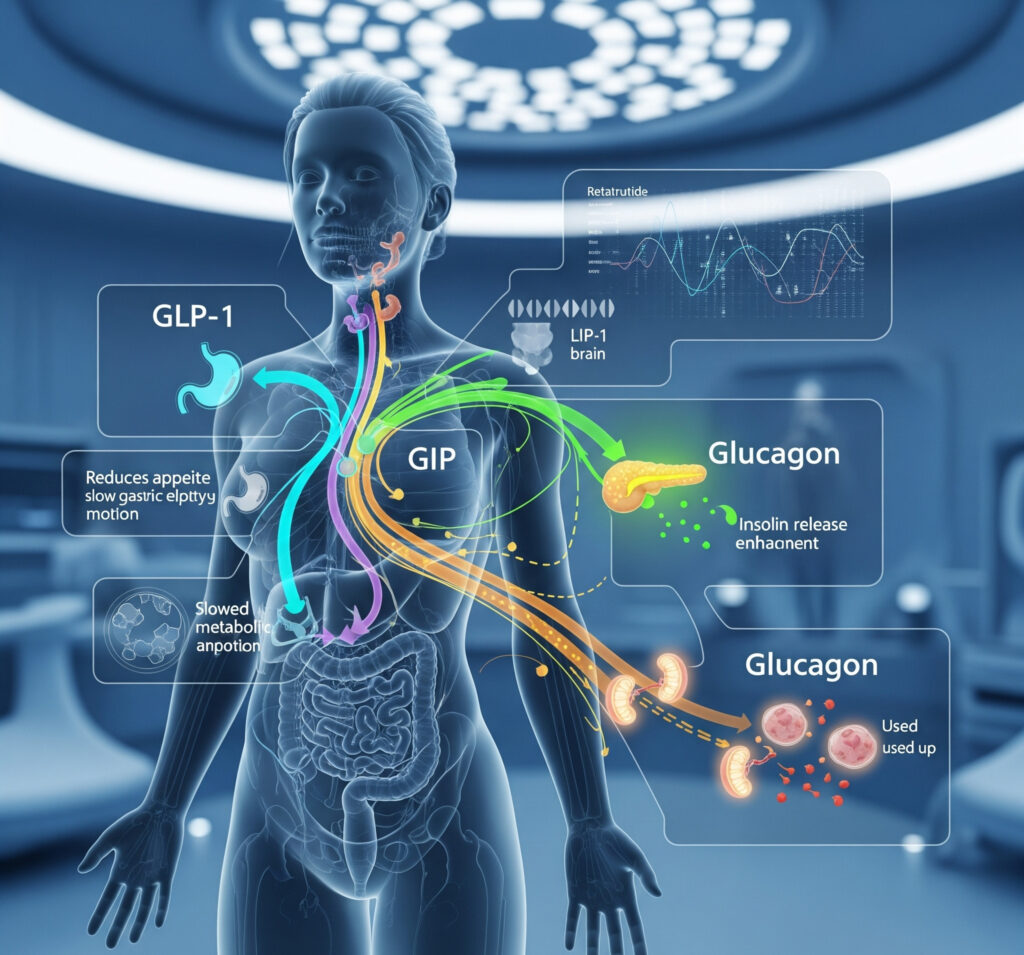
Individually, these pathways are powerful. But when combined, they create a synergistic effect that influences both sides of the energy balance equation: reducing calorie intake while increasing calorie expenditure.
This dual-action approach is one of the main reasons retatrutide is being described as a breakthrough in metabolic science.
Clinical Results and Weight Loss Potential
Early clinical trials have produced striking results. In Phase 2 studies, retatrutide demonstrated average weight loss of around 24% over 48 weeks, which is among the highest ever recorded for a pharmacological treatment.
More recent trial data has continued to support its effectiveness. Participants not only lost significant weight but also experienced:
- Improved blood sugar control
- Reduced visceral fat
- Better markers of metabolic health
In patients with type 2 diabetes, retatrutide has shown the ability to significantly lower A1C levels while continuing to drive weight loss over time.
Unlike some earlier drugs where weight loss plateaus, research suggests that retatrutide may continue producing results for longer durations, which could make it especially valuable for individuals with severe obesity.
Why Retatrutide Is Different
The key innovation behind retatrutide lies in the glucagon component. While GLP-1 and GIP primarily influence appetite and insulin, glucagon adds a third dimension: increased energy expenditure.
This means retatrutide doesn’t just help people eat less—it may also help the body burn more energy at rest.
This is a major shift from traditional approaches to weight loss, which typically rely heavily on appetite suppression alone. By targeting multiple systems simultaneously, retatrutide creates a more comprehensive metabolic reset.
Safety and Side Effects
Like all potent metabolic therapies, retatrutide comes with potential side effects. The most commonly reported issues in clinical trials include:
- Nausea
- Vomiting
- Diarrhea
- Gastrointestinal discomfort
These effects are similar to those seen with other incretin-based therapies, though they may be more pronounced at higher doses. There are also theoretical concerns related to glucagon activation, such as its impact on blood sugar levels, but current data suggests that the combined action of GLP-1 and GIP helps balance this effect.
Importantly, retatrutide is still investigational. It has not yet received full regulatory approval in most countries, and long-term safety data is still being collected.
Current Status and Availability
As of now, retatrutide is in Phase 3 clinical trials, with potential approval expected in the coming years if results remain positive.
Because it is not yet widely approved, it is not available through standard medical prescriptions in most regions. This has led to growing interest in research-grade versions, but this area exists in a regulatory gray zone and raises concerns about quality, dosing accuracy, and safety.
Medical experts strongly emphasize that therapies like retatrutide should only be used under proper clinical supervision once approved.
The Bigger Picture
Retatrutide represents a broader shift in how metabolic disease is being treated. Instead of focusing on a single pathway, modern therapies are increasingly targeting multiple systems at once—reflecting the complexity of human metabolism.
This multi-pathway approach may have implications beyond weight loss, including:
- Cardiovascular health
- Liver fat reduction
- Insulin resistance
- Long-term metabolic resilience
In this sense, retatrutide is not just another weight-loss drug—it’s part of a new class of therapies aimed at system-wide metabolic optimization.
Final Thoughts
Retatrutide peptide stands at the forefront of metabolic research, offering one of the most powerful combinations of fat loss, appetite control, and energy regulation seen to date. Its triple-receptor mechanism gives it a clear advantage over earlier treatments, and early clinical results are highly promising.
However, it’s important to balance excitement with caution. As an investigational compound, retatrutide still requires further study to fully understand its long-term safety and optimal use.
For now, it remains one of the most intriguing developments in modern medicine—pointing toward a future where metabolic diseases can be addressed more effectively than ever before.